U.S. employer health plan costs are projected to climb nearly 9% in 20261 — a sharper increase than in years past. For large companies, that means higher claims, tighter margins, and more pressure to make every healthcare dollar count.
To combat rising costs, companies may be tempted to reduce benefits offered. However, cutting coverage is rarely the right move. Instead, the most forward-thinking organizations are cutting waste — targeting the most avoidable cost drivers through proactive navigation, AI-powered tools, and better education around benefits. Here’s how they’re reducing their biggest healthcare line items without reducing access or quality.
What are the top 3 cost drivers in enterprise healthcare?
Enterprise healthcare costs are often not driven by a single factor, but by a convergence of three highly avoidable trends. Each trend stems from a lack of clarity, transparency, and proactive employee guidance.
Low-value care services
Redundant diagnostics, unnecessary MRIs, and excessive lab work are all too common. These services, while often necessary for diagnoses, may be recommended when other care pathways are more effective, carrying significant costs for both employees and employers. Without tools to compare quality or price, employees follow outdated referral patterns — driving up claims with no added benefit.
Out-of-network utilization
For large employers, out-of-network care is one of the most preventable sources of claims volatility and one of the least understood by employees. Many end up out of network without realizing it: referral defaults, outdated provider directories, or the assumption that “in-network hospital” means “in-network physician.” The result? A routine visit or procedure can cost 3 to 10 times more than expected.
At scale, these mistakes add up fast, especially in self-funded plans. Without smart navigation tools or real-time cost guidance, even well-designed benefits programs can hemorrhage spend from unintended out-of-network usage.
ER overuse
In large organizations, even routine healthcare decisions can create significant financial exposure. For non-emergency needs, many employees turn to the ER — not because it’s appropriate, but because it’s available. The absence of education around accessible telehealth or urgent care makes the ER the go-to option, even if those services are included in an employee’s plan. These unnecessary ER visits — according to a study by UnitedHealthcare — can cost between 15 and 52 times more than alternative sites of care.2
The common denominator across all three? A lack of clear, accessible information about the benefits package. When employees don’t know who is in-network, where to go for urgent needs, or how much services cost, they make decisions that unintentionally increase costs for themselves and for the organization.
The danger of overpaying for low-value care
Low-value care refers to services that drive up claims without delivering meaningful health outcomes. In enterprise plans, these often fly under the radar because they’re difficult to track without proactive analytics.
Common examples include:
- Unnecessary MRIs or CT scans performed without clinical justification
- Redundant bloodwork ordered by multiple providers who aren’t coordinating care
- Excessive lab panels that go beyond what’s needed for diagnosis or treatment
- Double-billing for services already included in bundled payments or provider contracts
- Routine testing performed more frequently than guidelines recommend
These services persist because employees don’t have easy access to second opinions, cost estimates, or context about whether a service is typical, necessary, or reimbursable. Many simply follow a provider’s suggestion, unaware that the same service may be unnecessary or available at one-tenth the cost elsewhere.
So how can enterprises identify and eliminate low-value care?
That’s where data and proactive design come in. By leveraging claims analytics, employers can pinpoint patterns of overuse and identify cost drivers across their population. These insights can spotlight gaps in care coordination, underutilized programs, and even outlier providers.
Case study: MRI pricing disparity and transparency gaps
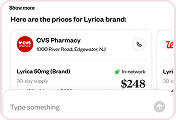
A recent example from a Healthee member illustrates the real-world cost of healthcare opacity. One member sought an MRI and was quoted $1,000 at a local hospital. By using Healthee’s AI assistant, they discovered a nearby imaging center offering the exact same scan for $40.
Results:
- Cost differential: 25x price difference for identical service
- Employee satisfaction: Improved by enabling informed decision-making
- Employer savings: Significant reduction in unnecessary claims exposure
This is not an isolated event. Price variability exists across nearly all geographies and procedure types. Without tools to navigate those disparities, employees (and by extension, employers) overpay for routine care.
Healthee’s impact: Directing employees to smarter choices
Here’s how Healthee helps large employers rein in runaway costs:
- Real-Time Navigation: Zoe answers care and coverage questions 24/7, helping employees compare prices, search in-network providers, and understand deductibles.
- Smarter Plan Selection: Our AI-powered plan comparison tool guides users during open enrollment, reducing costly plan mismatches.
- ROI at Scale: Enterprise clients have seen up to 7–14% reductions in claims costs within months of adoption.
- Lighter HR Load: Healthee slashes time spent on benefits questions, improves employee satisfaction, and gives HRs their time back.
Why AI-driven transparency is the new must-have
In large organizations, even small gaps in healthcare navigation can create outsized financial consequences. When employees lack access to clear, real-time benefits guidance, they default to decisions based on habit, provider referrals, or guesswork. This can, unfortunately, result in inefficiencies that compound across the workforce.
AI changes that.
Instead of forcing employees to decode PDFs or sit on hold with HR, AI translates messy, fragmented data — including EOBs, SBCs, eligibility files, and claims histories — into clear, actionable guidance. AI puts the most relevant plan, provider, and price details in front of employees at the moment they need them.
Critically, AI also delivers true medical cost transparency. Employees can compare prices for the same procedure across in-network providers, often revealing a 3–5x variation in costs. This level of visibility steers decision-making toward high-value care, protecting both employees and employer budgets.
At scale, the ROI is undeniable. Enterprises gain real-time insights into benefits utilization, identify emerging cost drivers early, and reduce the administrative burden on HR teams. This is the optimal (and we daresay, smarter) operating model.
Final thoughts for enterprise employers
The challenge for today’s enterprise leaders isn’t just managing rising healthcare costs; it’s doing so without sacrificing care quality, employee trust, or operational efficiency. That’s a high bar, especially when claims trends, inflationary pressure, and workforce expectations are all moving targets.
By targeting avoidable cost drivers like low-value care, out-of-network utilization, and ER overuse, leading employers are proving it’s possible to protect both the bottom line and the employee experience. And with the right infrastructure — AI-powered navigation, predictive analytics, and smart plan design — they’re scaling those wins across thousands of lives.
AI isn’t just a tool for efficiency. It’s a system of enablement. It helps HR teams operate more strategically, empowers employees to make confident, cost-effective decisions, and gives finance leaders the visibility they need to manage risk.
If you’re a large employer facing rising healthcare costs, don’t default to plan cuts. Default to smarter care access. Because in enterprise benefits, the path to savings doesn’t start with coverage reduction. With real-time tools, data-driven decisions, and AI-powered support, companies can control their largest healthcare costs while improving employee outcomes.
Sources
- WTW. “2026 Global Medical Trends Survey” https://www.wtwco.com/en-us/insights/2025/10/2026-global-medical-trends-survey
- United Healthcare. “Where employees seek care can impact cost and outcomes.” https://www.uhc.com/agents-brokers/employer-sponsored-plans/news-strategies/site-of-care