The benefits landscape is at a critical turning point. Following 15-year high premium increases and market-altering events like the FDA lifting the semaglutide shortage, HR leaders, plan sponsors, PEOs, TPAs, and advisors face unprecedented cost pressures heading into 2026.
In Healthee’s annual industry research report, we dive into the complex economic and policy shifts of 2025 that have defined today’s challenges, from changes to the ACA to the rising cost and demand of GLP-1 drugs.
Discover the context behind these trends to understand why navigating benefits has never been more challenging (and more vital) for controlling costs and supporting employees.

The healthcare and benefits landscape from 2025
HDHP + HSA: Prioritizing cost efficiency in plan designs
Building HDHP awareness and confidence
The other half: Making HSAs visible
Plan offerings across all types
Back to basics: Preventive care and maximizing utilization
What’s the benefit of preventive care utilization?
Focusing on long-term and mental health needs
Scrambling for savings: Handling high premiums in 2026
Dig into the demographics
Simplify benefits navigation and promote cost transparency
Make voluntary benefits more visible
Identify fraud, waste, and abuse
Rely on actionable AI claims analytics
Optimize point solution offerings
Squeezing savings throughout 2026
Benefits trends that are defining 2026
Multi-agent AI takes the lead
Appendix
The healthcare industry took many sharp turns in 2025. Premiums announced for 2026 had increased higher than most years in recent memory. The FDA lifted its shortage on semaglutide, sending GLP-1 costs and supply chains into a confusing wild west. A new presidential administration issued multiple healthcare-focused executive orders and spearheaded changes to Affordable Care Act (ACA) coverage, impacting private insurance markets in kind.
Despite the winds of change from 2025, I am hopeful about how 2026 is changing the benefits landscape. The team at Healthee has been bringing artificial intelligence (AI) to the healthcare and benefits experience for almost five years now. In that time, I’ve seen firsthand how the power of transparency and accessibility is transforming benefits experiences across the country. To me, it’s simple: When people can become confident, informed healthcare consumers, they can save precious time and money without sacrificing on quality.
In 2025, Healthee brought Zoe, our multi-agent AI assistant, to over one million U.S. households. And we’re watching as people discover the incredible ability of AI to help clarify benefits confusion and transform healthcare into an empowering experience. It’s these empowering experiences that we combed through to find some truly stand-out statistics that give me hope for healthcare.
We’re seeing the increasing adoption of HDHP plans and HSAs, driving medical savings that can compound over a lifetime. We’re watching people turn to preventive care and improve utilization of the benefits they — and their employers — are already paying for. We’re finding AI-powered cost transparency and care redirection delivering savings in an environment that’s otherwise increasing in cost.
AI tools like Healthee are bringing consistent, exponential value to the market in 2026. And I’m confident that we’ll see HR leaders, PEOs, brokers, TPAs, and the government alike turning to this latest technology for much-needed transparency and accessibility.
Guy Benjamin
CEO & Co-founder
at Healthee
Looking back at 2025, a lot of changes rocked the U.S. healthcare system and the employer-provided benefits ecosystem that layers on top of it. Before diving into the findings from Healthee’s 2026 Benefits Divide, let’s explore the context from which today’s trends arose. There are many avenues to explore, but these three events and circumstances had the biggest impact:
Healthcare premiums skyrocketed for 2026 during open enrollment in the fall of 2025. In the largest price hikes we’ve seen in 15 years, a 9% YoY increase in premium costs, these increases set the stage for a cost-focused year of benefits navigation in 2026.¹

The new U.S. presidential administration focused on several top-of-mind healthcare situations. First among them was changing the rules for ACA subsidies, leading to ACA premium increases which trickled down to private insurance markets. The current administration also issued a handful of executive orders targeting things like most favored nation drug pricing and healthcare price transparency.
In early 2025, the FDA lifted its shortage on semaglutide due to supply chain stabilization, directly impacting GLP-1 costs for consumers. Compounding pharmacies were resistant to give up profitable GLP-1 revenue, even after losing FDA protection. In response, drug manufacturers like Eli Lily and Novo Nordisk doubled down on direct-to-consumer channels for GLP-1 distribution through LillyDirect and NovoCare Pharmacy.
These changes also drove members of employer-sponsored plans to seek GLP-1 coverage through insurance, especially for weight management uses. Heading into 2026, there’s no sign of GLP-1 utilization slowing. About 10.5% of employer claims in 2025 were from GLP-1s.²
Each of these major policy and economic factors altered how Americans sought and used healthcare in 2025. And we saw how each of these elements impacted Healthee user behavior. Let’s dive into some of our 2026 Benefits Divide findings.
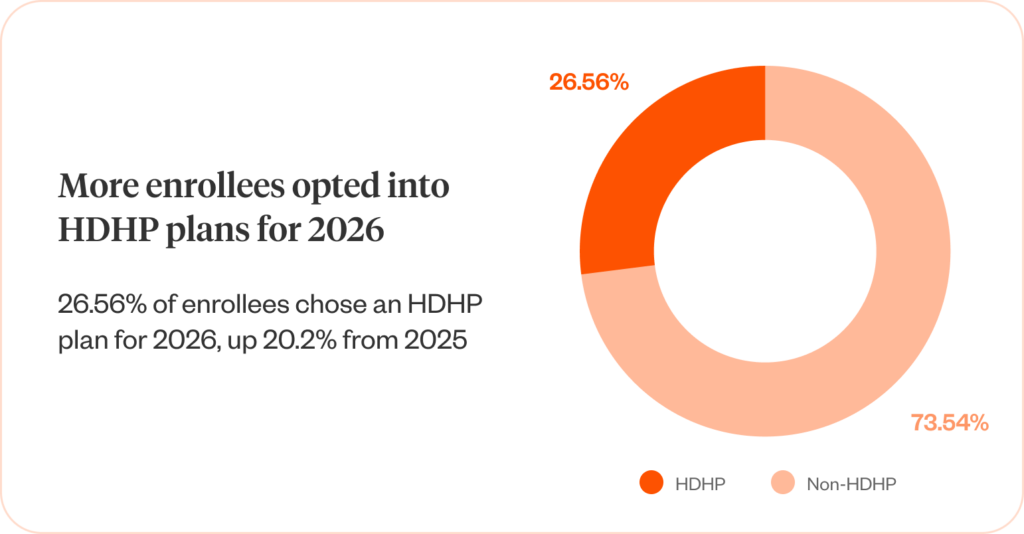
During open enrollment for 2026 plans, Healthee saw a significant portion of enrollees opt into high deductible health plans (HDHPs), many of which were eligible for health savings accounts (HSAs). This HDHP + HSA combo is a well-known mechanism for yearlong cost savings, both for the enrollee and their employer.
A few key elements led to this increase in HDHP and HSA adoption. By combining behavioral science and engagement tactics with hyper-personalized AI experiences, Healthee enabled thousands of organizations to dramatically increase awareness of HDHP and HSA opportunities.
By leveraging AI to help employees understand the value of HDHPs, Healthee saw a 20.2% year-over-year increase in HDHP selection. Further, Healthee users discovered and actively engaged in proactive education opportunities, learning about the value of HSAs with HDHPs, leading to a 42% year-over-year increase in HSA adoption among eligible enrollees.
But we found that education alone isn’t enough. With the support of dynamic HSA financial modeling, 35% of Healthee enrollees selected the maximum IRS-allowed HSA contribution amount.
Healthee works with incredible organizations across the U.S. offering HDHP plans. But we’ve seen time and again that our clients want better HDHP adoption. With a leading U.S. social media company, Healthee’s AI-powered Plan Comparison Tool experience drove a +50.1% increase in HDHP enrollments in 2025 from the previous year.
By providing proactive education, enrollees can make confident, cost-effective enrollment choices regardless of prior knowledge or enrollment behaviors like only opting into familiar PPOs. But employees can’t choose HDHPs alone — they need buy-in from their employers to even offer these plan options in the first place.
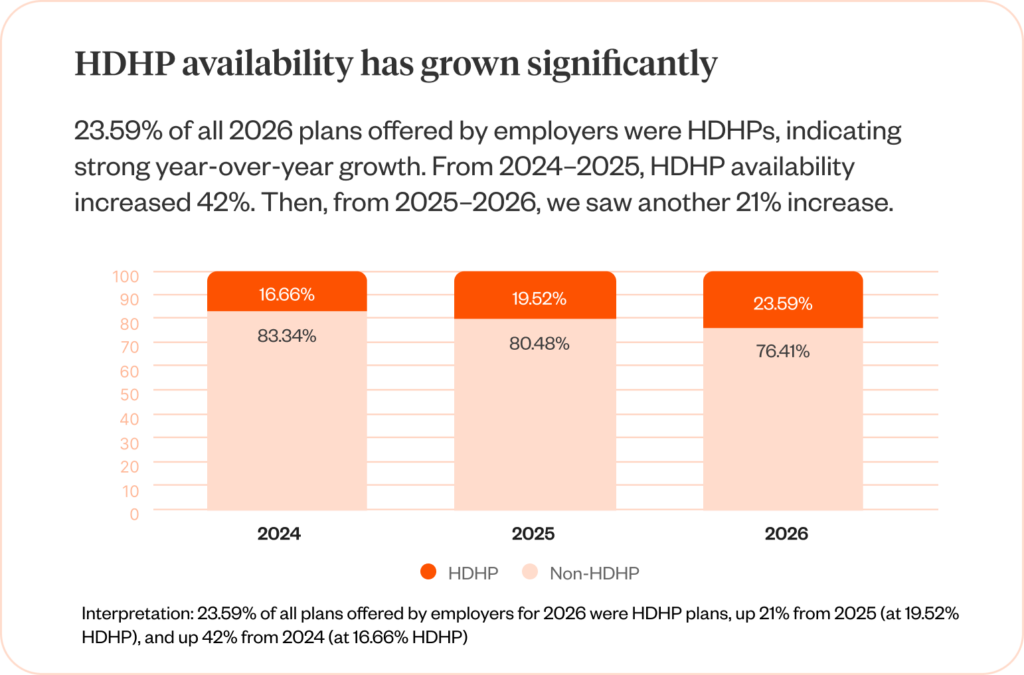
In an encouraging turnaround, Healthee saw a 21% year-over-year increase in the number of HDHP plans offered by employers from 2025 to 2026. In the 2025 Benefits Divide, we discussed how limited HDHP availability led to lower enrollment. By increasing the availability of HDHPs, we observed a direct correlation with higher HDHP enrollment.
Looking ahead to 2026, 54.56% of enrollees indicated that they expected to have medium to high medical needs in the coming year. That’s more than half of the enrolling population anticipating significant reliance upon their selected benefit plans.
In a year where premiums skyrocketed, showing the value of financial savings has never been more urgent. A significant portion of Healthee users opted into health savings accounts (HSAs), showing the viability of such financial opportunities to enrollees in 2026 plans.
Healthee users discovered and actively engaged in proactive education opportunities, learning about the value of HSAs with HDHPs, leading to a 42% year-over-year increase in HSA adoption among eligible enrollees. For one client, a large national health system with over 80,000 employees, Healthee’s PCT nearly doubled HSA enrollment to 45.1% of eligible employees, a +15 percentage point shift from the previous enrollment period before Healthee.
With the support of dynamic HSA financial modeling, 35% of Healthee enrollees selected the maximum IRS-allowed HSA contribution amount. As we enter 2026, we can expect these enrollees to double down on the triple-tax-advantaged savings of health savings accounts.
“An HDHP paired with an HSA gives employees something truly powerful: agency over both their health and their financial future. For many, especially younger generations who are thinking strategically about long-term savings, this combination lowers costs today while building a portable, tax-advantaged cushion for tomorrow’s bigger healthcare moments. It’s one of the most financially sound choices employees can make. A way to invest in their wellbeing now, protect their future selves, and carry that security with them wherever their career takes them.”
Elle Meza, Advisor & Consultant, Elle Meza Consulting
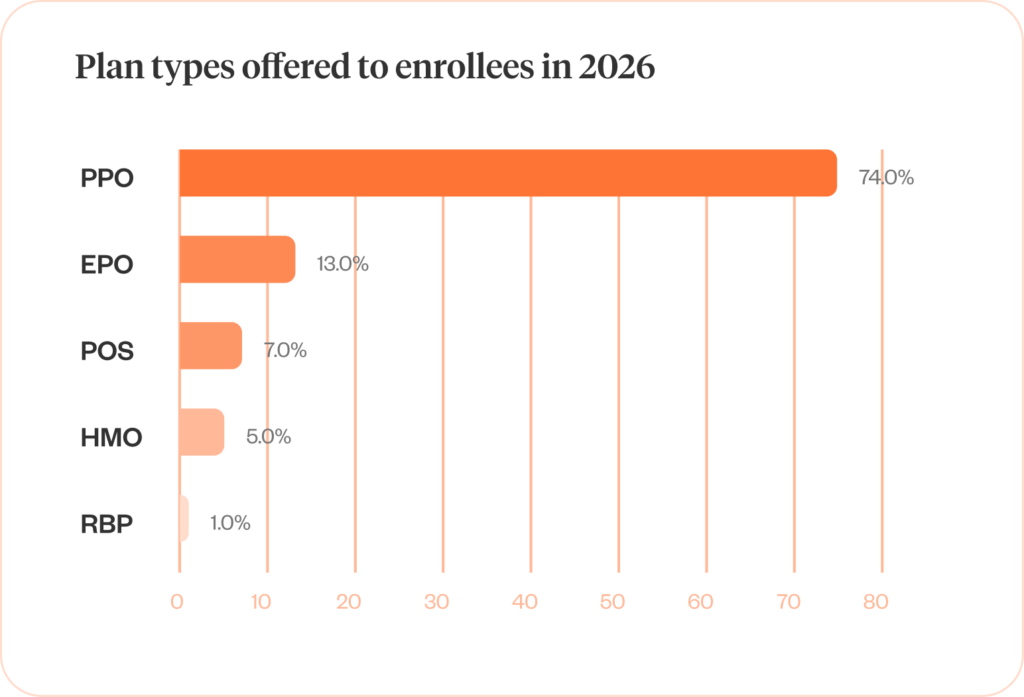
Let’s zoom out from HDHPs and HSAs alone. When looking at the entire spread of plan types offered through our PCT for 2026, we saw a similar breakdown to last year. Unsurprisingly, PPO plans dominate the market at 73.61%, showing this higher-cost, higher-coverage option still appeals to a large portion of the enrolling population.
In a far second are EPO plans at 12.67%. These plans work in the middle space between PPOs and HMOs, but with much narrower networks and higher out-of-network penalties. While we’re seeing an increase in novel, cost-effective plan designs with the increase in HDHP offerings, we’re seeing a relatively low and stagnant exploration of additional creative plan designs like RBP and ICHRA.
Looking back at 2025, Healthee users searched for a lot of medical care. But a few categories stood out from the rest. In fact, the top 10 most common care categories searched fell into two buckets: preventive care and smart utilization.
Top 10 care categories for 2025
1. Annual physical (9.35%)
2. Chiropractor (5.80%)
3. PCP visit (5.67%)
4. Dental cleaning (4.08%)
5. Eye exam (3.95%)
6. Weight management (3.43%)
7. Dermatologist (3.29%)
8. Psychotherapy (2.90%)
9. Physician (2.90%)
10. MRI scan (2.90%)
Of all 326 care categories identified for 2025 searches, annual physicals topped the list at 9.35%. In fact, search volume for “annual physical” was 61% larger than the second category on the list, “chiropractor.” Our take? People are searching for preventive care like never before. Doubling down on the preventive care group, “pcp visit,” “dental cleaning,” “eye exam,” “dermatologist,” and general “physician” accounted for 60% of the top 10 categories in 2025.
The healthcare industry should feel encouraged that the majority of healthcare navigation last year was in search of preventive care. That means more people getting more routine care, detecting chronic diseases early, and building positive healthcare habits. As people search for more preventive care, they’re also eking out the most value from their benefit plans, showing that opportunities for clear benefits navigation lead to preventive care discovery.
“Preventive care becomes life-changing when someone finally feels seen, guided, and supported. Connecting people to the right provider, giving them clear steps, and offering real access turns fear into confidence—and health into something they can protect.”
Susana Villegas Spillman, HR and Benefits Executive, Abbott
Preventive care is one of the most effective methods for improving long-term health outcomes and reducing healthcare costs. When employees access preventive services — such as annual physicals, cancer screenings, immunizations, and wellness visits — they’re more likely to catch health issues early, when treatment is simpler and less expensive.
Preventive care utilization means catching cancers earlier, exploring weight management solutions before diabetes onset, and pursuing treatment for chronic allergy symptoms. Depending on the plan type, preventive care also serves as the conduit to specialist services. For those on HMO plans, their PCP needs to provide a referral in order for them to further navigate their healthcare.
Or imagine those on HDHPs who are typically healthy and chose an HDHP because they had low anticipated healthcare utilization in the coming year. These people still need to complete annual physicals and maintain dental and vision health year to year. No matter the plan type, patient age, or medical need, preventive care in 2026 is essential for yearlong benefits management success.
“Preventive care is most effective when employees know where to start and feel supported along the way. When information is clear and guidance is easy to follow, people are more likely to take action early, whether that means scheduling routine screenings, addressing concerns sooner or making healthier choices before issues escalate. Simplifying the experience reduces hesitation and confusion, allowing preventive care to become part of everyday decision making rather than something employees put off. Over time, this proactive approach leads to healthier employees and more meaningful use of benefits.”
Nelissa Arriaga, Senior Manager, Global Benefits, Celonis
Now, turning to the other bucket of smart utilization. The rest of the top 10 show how people are searching for high-value non-preventive care opportunities like “chiropractor,” “weight management,” and “psychotherapy.” Whether Healthee users were getting their back cracked by a chiro or finding mental health support, it’s unsurprising that people were looking for opportunities to manage long-term health needs.
Another theme within these top ten care categories and beyond is mental health. Employee demand for mental health support will only continue to grow into the future. As their demand grows, organizations must meet them with effective tools for navigating mental health benefits and finding the right care. Navigational tools that identify cost-effective talk therapy options will be especially crucial as the pool of in-network therapists shrinks.
“Mental health support is an essential part of every benefit plan. Employees need to know that they’re covered for services like talk therapy and psychiatry. But without clear benefits navigation experiences, these insurance-covered options fall out of sight. Organizations that want to help their people find ways to improve their mental well-being in 2026 will opt into solutions that make these care opportunities visible. Seamless access to tools like 24/7 telehealth therapy, psychiatrist lookup, and mental health point solutions can go a long way.”
Jake Schwartz, VP of Client Services, Healthee
As we look ahead to the 2026 plan year, continue encouraging members to engage in preventive care, discover mental health support, and pursue opportunities for proactive early detection.
3 reasons why premiums skyrocketed in 2026
The U.S. healthcare system is always in flux. One of the largest changes that impacted a significant swath of enrollees for the 2026 plan year was 15-year-high premium increases. As enrollees stare down their exponentially high monthly premiums, let’s take a minute to understand how we got here:
1. The first and more prominent reason for higher premiums in 2026 was the expiration of enhanced premium tax credits within the Affordable Care Act (ACA/Obamacare), which led to plan designs with higher out-of-pocket costs for enrollees. The resulting worsening risk pool then drove up average claims costs across the ACA marketplace and the private insurance market. This public-private ripple effect has driven up costs for everyone, regardless of plan type or plan sponsor.
2. Another unignorable aspect of high premiums is the overall economic landscape, including rising inflation, tariffs on imported pharmaceuticals and medical supplies, and the corresponding increased labor costs hitting healthcare facilities (who then pass those new costs on to consumers).
3. Thirdly, as GLP-1 prices continue to become a larger portion of claims volume (upwards of 10%), plan sponsors and members will bear increased cost per dose amid increasing demand.

Higher premiums don’t have to spell financial stress for plan sponsors.
During enrollment for 2026 plans, Healthee discovered several key demographics that could benefit from more targeted outreach and proactive communication through the coming year. Healthee’s open enrollment decision support platform includes a robust intake process. Our Plan Comparison Tool (PCT) allows enrollees to self-report their expected medical needs for the coming year in order to find the best-fit benefit plans.
Looking ahead to 2026, 54.56% of enrollees indicated that they expected to have medium to high medical needs in the coming year. That’s more than half of the enrolling population anticipating significant reliance upon their selected benefit plans.
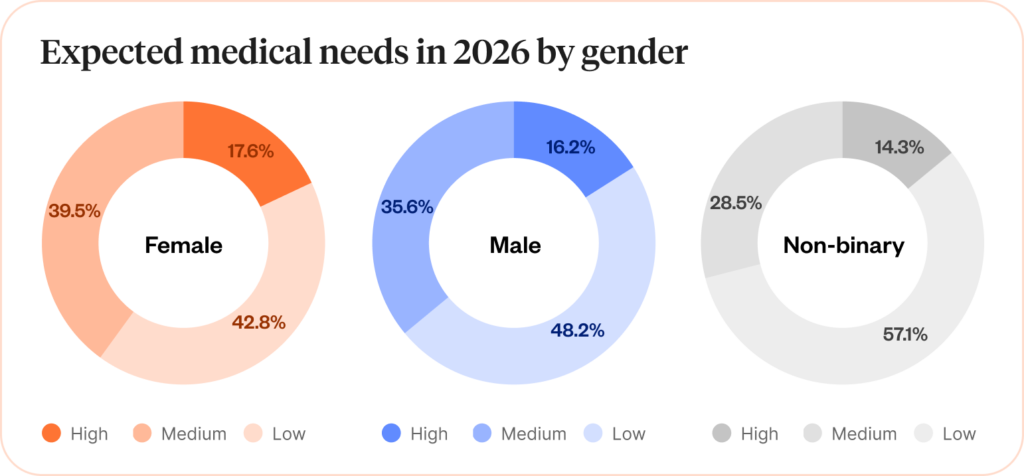
Drilling further down by gender, 57.18% of female enrollees indicated medium to high expected medical needs, compared to 51.8% of male enrollees. This 5.38 percentage point difference reveals a unique opportunity. When factoring in the non-binary population, this group self-reported comparatively lower anticipated health needs.
As employers look for employee subgroups for targeted health interventions, our data indicated they should focus on their female employees and their coming health needs in order to mitigate costs.
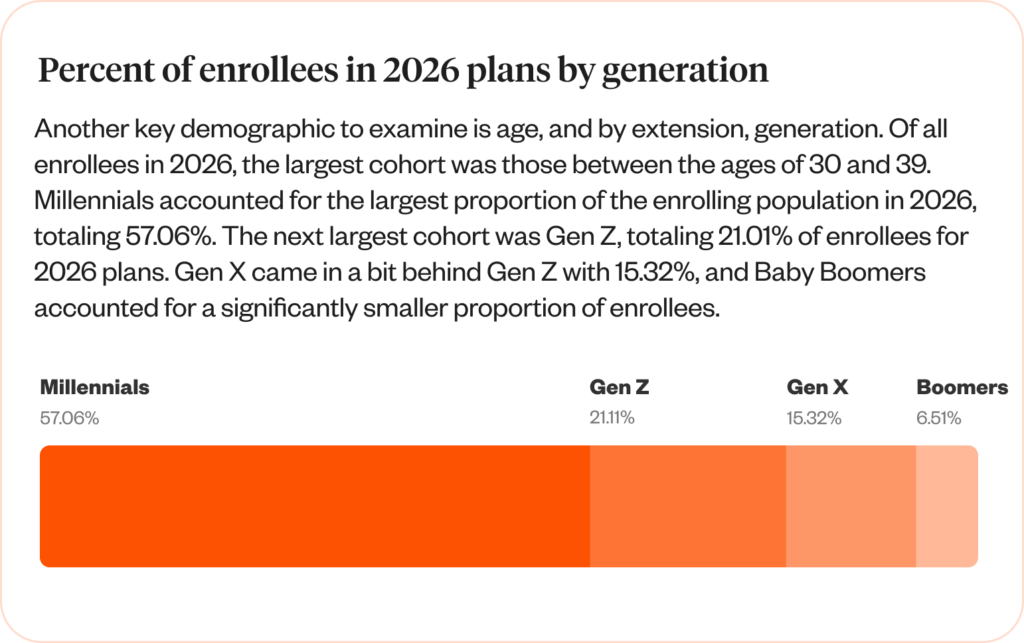
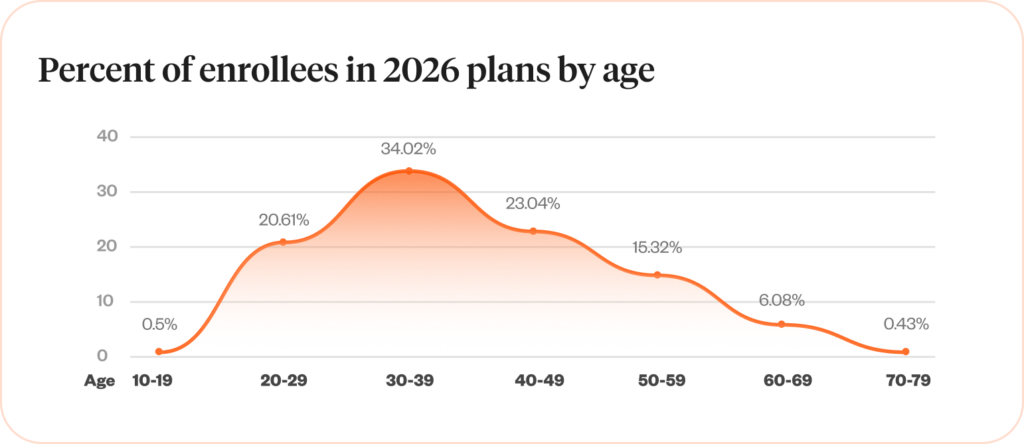
The generational breakdown in enrollees reflects the wider shift in workforce demographics. Baby Boomers are retiring or electing into government-sponsored plans, effectively disappearing from the private health insurance market as a whole. Gen X is similarly retiring and making up a smaller portion of the insured public.
Given that Millennials make up more than half of all enrollees in 2026 benefit plans, it would be prudent for organizations to target this population, especially as they enter a new era of preventive care needs such as colonoscopies and more frequent cancer screenings.
“The generational challenge in benefits isn’t age, it’s cognitive load. Today’s workforce spans digital natives and analog decision-makers, each processing information differently, often under stress and time pressure. HR leaders who design benefits communication as an adaptive experience (much like the ones partnered and offered with Healthee) remain personalized, on-demand, and context-aware; moving employees from passive exposure to confident benefit decision-making.”
Erica Morrison, Total Rewards and Analytics Manager, BeatBox Beverages
This year also marks a high percentage of Gen Z enrollees, offering a unique opportunity to support those who are newer to health insurance. With over 21% of 2026 enrollees being digital-native, insurance-unaware Gen Zers, this population is ripe for proactive support and AI-powered benefits navigation tools.
And, benefits leaders must also be considering the rising Gen Alpha cohort. The older Gen Alphas will will join the workforce in the next one to three years, with the full force of this generation coming in the early 2030s. As we plan for the benefits landscape for the next five years, it’s imperative to explore ways to improve this generation’s entrance to the benefits enrollment experience.
Much as AI has improved, digital-native generations like Gen Z and Gen Alpha will expect an even more technologically adept ecosystem for healthcare and benefits management. If we’re going to effectively serve these future populations, we must start building and implementing the best tools now, before their first benefits enrollments.
“To truly connect with today’s multigenerational workforce, we have to abandon a ‘one-size-fits-all’ approach and shift toward an equitable, responsive, and accessible model of benefits that meets people where they are. This means balancing mobile-first, bite-sized, self-service content for digital natives with large-group, general overview presentations and targeted 1:1 deep dives for individuals preferring a more human touch. Our call to action is to raise our awareness that each audience may need a different approach to recognize value in the benefits offered and to curate a variety of means to access those resources.”
Korey Reynolds, Sr. Director of HR, 10,000 Degrees
Another way to explore the data is to understand where your employees are located across the country. While you may have this data floating around your HRIS, it’s worth understanding where the majority of 2026 enrollees are geolocated.
Across Healthee’s user base, we saw the most 2026 enrollees in California, Minnesota, and New York. As you look ahead to 2026, consider if you also have a similar distribution of employees. While organizations shouldn’t ignore states with fewer employees, state-based interventions could go a long way toward better supporting your people.
For example, if your employees are more densely located around major city centers, you have a perfect opportunity to implement a cost transparency solution to help them find the best-priced care in a sea of options. Or, if your employees are more distributed across semi-rural and rural areas with more limited access to healthcare, consider implementing solutions like 24/7 free-to-use telehealth that can reach where in-person physicians can’t.
Top 10 states with the most 2026 enrollees
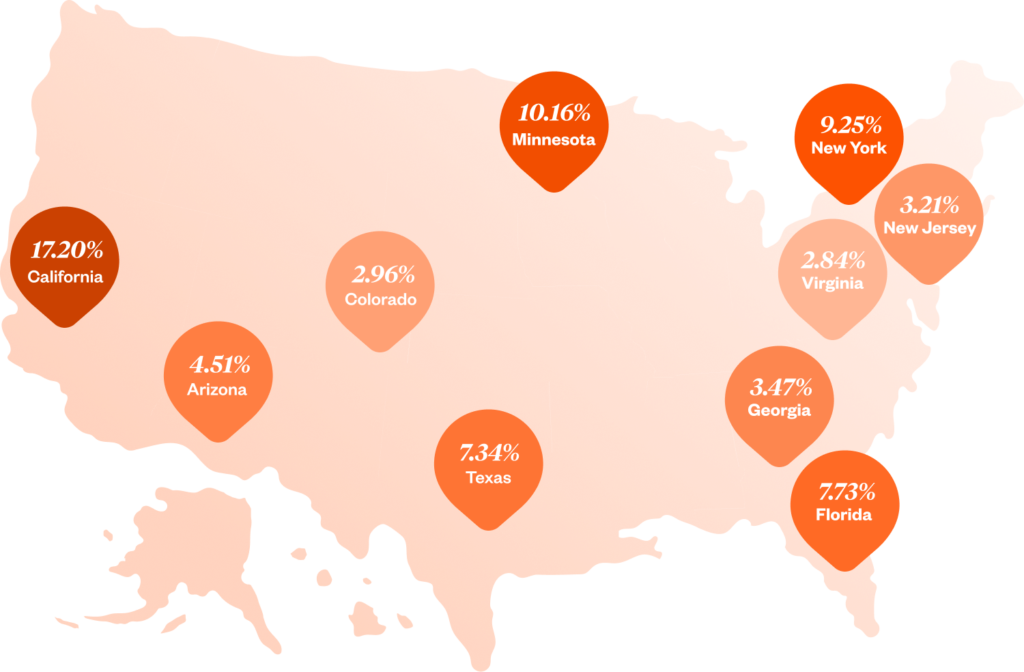
How can you combat high costs? By creating a market with equal footing between consumer and provider.
The U.S. healthcare system has been opaque for far too long. With the application of the latest AI-powered technology, benefits navigation has become even better at helping people find the lowest cost care near them. By providing personalized navigation experiences, platforms like Healthee are empowering everyday Americans to become better healthcare consumers. Simply put, cost transparency is helping people save money every day. Full stop.
Healthee is your people’s one-stop shop for all things benefits and healthcare navigation. As your people understand, explore, and utilize their benefits throughout the year, make sure they have an AI-powered tool in their back pocket.
“It’s never been more important for HR leaders to step in and support Gen Z and Millennial employees. This population accounts for over 78% of all people using employer-sponsored benefits in 2026. Both generations are tech-savvy and information-hungry, making them the perfect candidates for the latest AI-powered benefits navigation tools. By providing cost transparency, agentic AI assistance, and benefits education at scale, I firmly believe that organizations can curb the 15-year high healthcare costs throughout the year.”
Debbie Sharvit, VP of People, Healthee
Voluntary benefits (VBs) present a fundamental challenge for today’s organizations: despite significant investment in comprehensive benefit offerings, enrollment rates remain disappointingly low. Employees struggle to understand the value of supplemental coverage, while HR teams lack the bandwidth to provide personalized guidance at scale.
This disconnect is costly. Employees miss out on crucial financial, legal, and personal protection. Employers see minimal return on their benefit investments. Brokers leave commission dollars on the table. But what if there was a better way?
At Healthee, we’ve found that AI-powered decision support helps employees not miss out on important VBs and transforms confusion into confidence, turning voluntary benefits from an afterthought into an essential component of comprehensive employee protection.
Organizations using Healthee’s Plan Comparison Tool for 2026 enrollments achieved a remarkable milestone: 71.2% of eligible users saved one or more voluntary benefit plans. By coupling AI-powered decision support with behavioral science, proactive nudges, clear education, we saw a fundamental shift in how employees engage with benefits.
As you plan your 2027 enrollment, consider how you can boost voluntary benefits visibility to the right eligible employees at the right time. Enrollees in 2027 plans will be fresh off the heels of a year of high-cost healthcare. By surfacing the right opportunities for additional cost savings, organizations can help match enrollees with high-quality VBs.
Fraud, waste, and abuse (FWA) is rampant throughout the U.S. healthcare system. Unfortunately, the financial burden is often borne by the plan sponsors who foot the bill without access to the analytics they need to recoup those lost dollars.
Organizations looking for innovative solutions to the 2026 healthcare financial challenges should explore FWA services. At Healthee, we’ve helped a global technology manufacturing company identify over $10.6M in suspicious claims in 2025 through our AI-powered FWA team. Here are a few FWA scenarios you can look out for in 2026:
As finance leaders across organizations look for ways to mitigate higher claims costs in 2026, FWA services are a surefire way to identify opportunities for recouping funds.
Every organization is in a different place when it comes to their claims data. Some experience challenges with their vendors and lack explicit visibility into their deidentified claims data. Some self-insured employers may have crystal clear access to their claims data.
But what if you could go beyond simply looking at claims charts and admiring how far they’re going up and to the right? Actionable AI claims analytics is the next tool in your financial toolbox for paring down on excess plan spend.

Agentic AI tools on the market today constantly scan your claims data for savings opportunities and proactively surface those opportunities without human intervention. Do you have a high volume of mental health claims coming through that could be mitigated with a targeted point solution?
Well, an AI agent can help you interpret your claims data to find out and lead you to the next best step.
Point solution fatigue has already come and gone. But the problem isn’t the availability of point solution offerings; it’s the lack of visibility and navigational opportunities surrounding them.
When members have clear, actionable ways to engage with employer-provided point solutions, engagement and utilization problems disappear. In fact, the most-clicked benefit opportunities in the Healthee platform in 2025 were Healthee Perks point solutions like LifeMart discount programs and Hims & Hers.
As you consider point solutions in 2026 and beyond, here’s a breakdown of the most popular point solution offering types across the Healthee ecosystem:
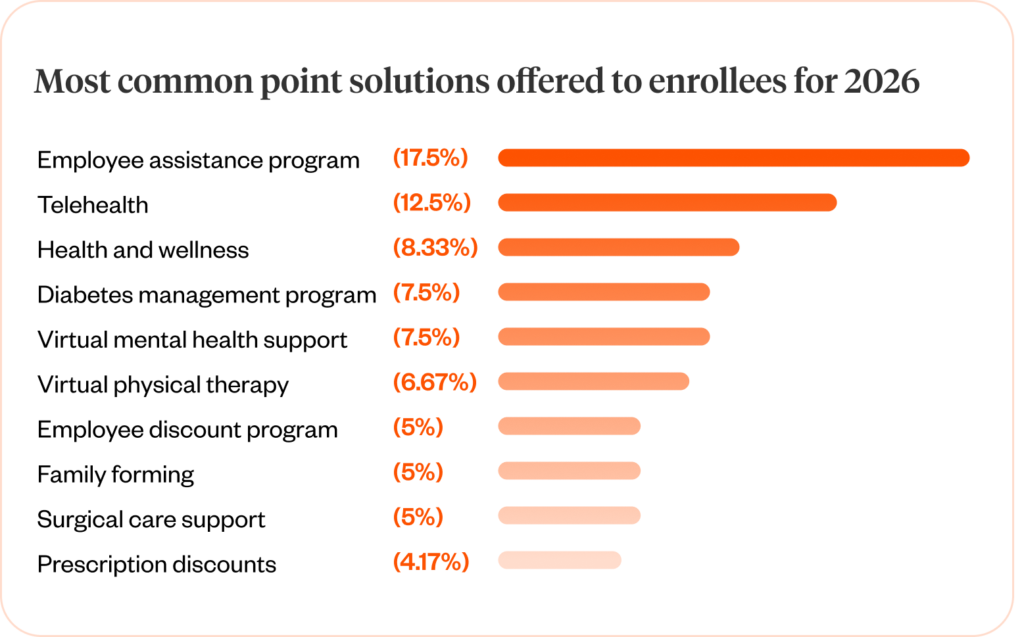
In sum, here are the best and most effective ways you can reduce plan spend and help your people save on healthcare costs in 2026:
1. Employers are figuring out how to manage the high costs of GLP-1s
Increased adoption of GLP-1 coverage by employer-sponsored plans will have secondary impacts like increased talent retention and attraction. Weight management was the 6th most-searched care category in 2025. Healthcare leaders can expect even more GLP-1 exploration in 2026.
2. Increased HDHP adoption with supplemental HSA utilization will support lower claims costs for employers and greater wealth accumulation for enrolled employees at larger scale than before
Backed by the fact that younger demographics are using HA less through the year compared to middle-aged and older adults. If these people have been steered to the more cost-effective HDHP plans, they’ll be able to generate savings. Furthermore, employees who have opted into HSA with their HDHP plan will continue to generate triple-tax-advantaged savings. When costs are front and center for 2026, long-term savings will be even more appealing.
3. Preventive care utilization will continue to increase in 2026 driven by:
Positively: Increased benefits visibility through navigational tools like Healthee.
Negatively: As care costs increase for non-preventive services, covered preventive services will be more cost-effective alternatives.
4. Anticipated medical needs will be met with enhanced navigational support
More than half (54.56%) of enrollees for 2026 anticipated medium to high expected medical needs. These people are likely to be managing chronic diseases, navigating pregnancies, and utilizing care at higher rates during the 2026 plan year. These people will need ways to save money amid the rising healthcare costs, pushing the need for and utilization of AI-powered benefits navigation like Healthee.
5. Mental health will continue to be top-of-mind for employees as they utilize their benefits and search for in-network therapists
The #8 (psychotherapy) and #11 (mental health therapy) most-searched care categories for 2025 are related to mental healthcare. Employees will continue to utilize this employer-provided mental health services and use navigational tools to identify cost-effective talk therapy options as the pool of in-network therapists shrinks. And with increased visibility into available point solutions, targeted mental health needs will be met at higher rates.
As we experience the 2026 plan year and build 2027 benefit strategies, it’s worth remembering the largest benefit trend on the horizon: artificial intelligence.

In the realm of AI, 2025 was the year that agents took center stage. In 2026, multi-agent AI and agent-to-agent (A2A) management will be the top-line discussion across industries.
As healthcare and benefits leaders approach multi-agent AI and A2A, it is as important as ever to consider how your vendors are implementing member-facing AI. Regulatory requirements and HIPAA safeguards are just the start — multi-agent AI introduces a whole new world of technological opportunity (and pitfalls if handled poorly).
At Healthee, we’ve seen a massive change in the tides from AI hesitancy to AI adoption across the industry. Artificial intelligence has become an expected facet of modern benefit technologies. And we are leading the charge with our best-in-class multi-agent AI assistant, Zoe.
Whether you’re building A2A frameworks for internal AIs in 2026 or you’re relying on vendors to build agentic AI for your people, benefits experts must be on the lookout for the safest and most advanced AIs on the market.
Throughout our research for the 2026 Benefits Divide, one core message rang true: Costs are on everyone’s minds. From plan sponsors to TPAs to PBMs to patients, every actor in the U.S. healthcare system is keeping an eye on just how expensive this new year of benefits and healthcare utilization will be.
Benefits in 2026 are more complex than ever. Industry experts need to rely on clean, actionable data and agentic AI experiences to contain skyrocketing costs. Organizations that launch multi-pronged AI cost containment strategies will find themselves ahead of the curve.
When it feels like everyone is staring down the barrel of elevated healthcare costs, we cannot forget the levers at our disposal:
If you’re looking to pull one of these levers in 2026 or beyond, Healthee is the leading multi-agent AI platform on the market, with proven technical solutions for each of the leading challenges for benefits in 2026.
The 2026 Benefits Divide utilizes proprietary data collected by Healthee’s Data Science team from internal sources between January 1, 2025 and December 31, 2025. All trend analyses were rigorously vetted to ensure accuracy. In compliance with HIPAA regulations, the report contains no personal health information (PHI); all data have been de-identified to maintain confidentiality and uphold the highest standards of data privacy.
Thank you to all contributors to The 2026 Benefits Divide, including the thought leaders from across the health and benefits industry who shared their invaluable insights, including:
Guy Benjamin, CEO & Co-founder, Healthee
Debbie Sharvit, VP of People, Healthee
Jake Schwartz, VP of Client Services, Healthee
Elle Meza, Advisor & Consultant, Elle Meza Consulting
Susana Villegas Spillman, HR and Benefits Executive, Abbott
Nelissa Arriaga, Senior Manager, Global Benefits, Celonis
Erica Morrison, Total Rewards and Analytics Manager, BeatBox Beverages
Korey Reynolds, Sr. Director of HR, 10,000 Degrees